A Hyperpigmented Right Forearm
History
An 18-year-old female returned from Mexico and was concerned about the hyperpigmentation on her right forearm. Two weeks earlier, lime juice was accidentally squirted on her forearm during a barbecue on a sunny beach in the Bahamas. By the following morning, a burning sensation and erythema were noted in the affected forearm. Ten days later, the erythematous area became hyperpigmented.
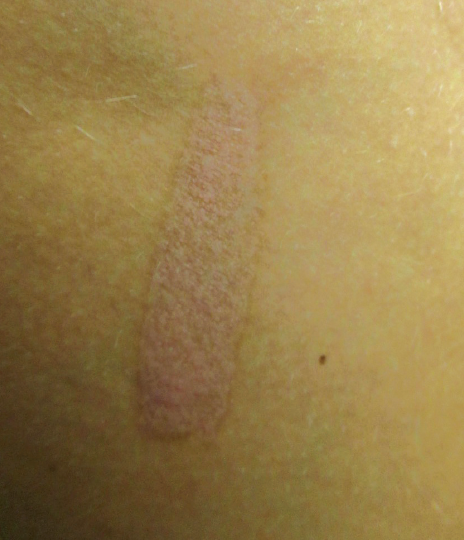
PHYSICAL EXAMINATION
Physical examination revealed 2 well-demarcated hyperpigmented patches on the flexor aspect of the right forearm and the medial aspect of the right elbow, respectively.
What’s Your Diagnosis?
A. Irritant contact dermatitis
B. Polymorphous light eruption
C. Porphyria cutanea tarda
D. Bullous pemphigoid
E. Phytophotodermatitis
(Answer and discussion on next page)
Answer: Phytophotodermatitis
Phytophotodermatitis refers to a nonimmunologic photosensitive dermal reaction induced by the contact to or, very rarely, oral intake of a photosensitive substance found in certain plants followed by exposure to sunlight.1 Robert Klaber in 1942 coined the term phytophotodermatitis to describe the phenomenon.2 Some people have since referred to it as “Club Med” dermatitis.
Epidemiology
The exact incidence is not known as information on this condition is limited to case reports. Phytophotodermatitis is most commonly seen in the summer when furocoumarins are at the highest concentrations in plants, when people are outdoor more often with less protective clothing, and when ultraviolet exposure is greatest.3,4 Perspiration, high humidity, and heat increase the absorption of furocoumarins, thereby increasing the intensity of phototoxic reactions. Phytophotodermatitis is observed more frequently in individuals who spend a lot of time participating in outdoor activities.4 There is no predilection for race, sex, or age, but the condition is most easily recognized in fair-skinned individuals.3
___________________________________________________________________________________________________________________________________________________________________________________________________________________
RELATED CONTENT
What could cause this pigmentation on her wrist?
Why the onset of an itchy eruption on her neck?
__________________________________________________________________________________________________________________________________________________________________
Etiopathogenesis
Phytophotodermatitis results from the interaction of solar radiation and photosensitizing compounds in various plants. Furocoumarins—such as psoralens, 5-methoxypsoralens (bergapten), 8-methoxypsoralens (xanthotoxin), angelicin, pimpinellin, limettin, and bergaptol—are commonly implicated.4 The most common plant families high in furocoumarin content and capable of provoking phototoxic reactions are Rutaceae (eg, limes, lemons, oranges, tangerines), followed by Umbelliferae (eg, parsnips, parsley, celery, carrot), Moraceae (eg, figs), and Leguminosae (eg, legume, pea, bean).3-5 The wavelengths of ultraviolet light that most effectively produce phytophotodermatitis lie within the ultraviolet-A 320 nm to 400 nm range, and have peak activity at 335 nm.4
After the furocoumarins are exposed to ultraviolet radiation, they form phototoxic compounds that cause direct damage to the DNA of epidermal cells. Two types of phototoxic reactions are recognized. Type 1 is oxygen independent, in which the ultraviolet-activated furocoumarins bind to RNA and nuclear DNA.6,7 This results in interstrand cross-linking with inhibition of DNA synthesis. Type 2 is oxygen-dependent, where ultraviolet-activated furocoumarins cause damage to epidermal, dermal, and endothelial cell membrane in addition to intracellular enzymes, RNA, and DNA.6-8 These reactions lead to apoptosis of keratinocytes, which manifest clinically as erythema, edema, and bulla formation.8 Subsequent hyperpigmentation is caused by type 1 reaction and results from increased melanocyte mitosis and dendricity, melanocyte hypertrophy, increased tyrosinase activity, increase in number of melanosomes in melanocytes, and migration of melanocytes from the epidermis to the dermis.3,6-8 Less commonly, hypopigmentation may result and is attributable to apoptosis of melanocytes.7
Histopathology
Histopathologic examination of a classic lesion in the acute stage shows spongiosis, vacuolization, and keratinocyte necrosis.4 Later on, intra- and subepidermal blistering may be seen.
Clinical Manifestations
A phototoxic inflammatory eruption typically occurs 24 hours after the exposure of the skin to a furocoumarin and sunlight, with a peak at 30 to 120 minutes.1,6 Clinically, this is manifested as bizarre configurations of erythema with a sharply demarcated border confined to the area that has come in contact with the offending plant agent and consequent sun exposure. A burning sensation and pain are prominent. Vesicles and bullae may develop after 24 hours and peak at 72 hours, and often accompanied by subsequent desquamation and denudation.6 Pruritus does not seem to be common.
Hyperpigmentation often develops 1 to 2 weeks later and can appear in bizarre streaks or drop-like patterns where the furocoumarin contacts the sun-exposed skin.6 Less commonly, hypopigmentation may result.4 Phytophotodermatitis is most commonly seen on uncovered sites exposed
to sunlight and plants such as arms and legs.
Diagnosis
The diagnosis is a clinical one. Key elements are taking a history of exposure to a plant followed by sunlight exposure and familiarity in recognizing the clinical appearance of the lesion (typically linear). A skin biopsy should be considered if the diagnosis is in doubt.
Photopatch testing is not recommended because a positive response can be very severe.9 Referral to a dermatologist should be considered if there is diagnostic uncertainty.
Differential Diagnosis
Differential diagnoses include irritant contact dermatitis, allergic contact dermatitis, polymorphous light eruption, sunburn, chemical or thermal burn, herpes simplex, herpes zoster, child abuse, factitious dermatitis, atopic dermatitis, porphyria cutanea tarda, and bullous pemphigoid.5,10
Complications
Rarely, the hyperpigmentation may be permanent and scarring may occur.
Prognosis
The prognosis is good. The hyperpigmentation or hypopigmentation usually lasts for several months to a year. Resolution of the hyperpigmentation can be hastened with proper sun protection and bleaching creams.7
Prevention
If contact with relevant plant or known photosensitive compounds is suspected, the exposed skin should be thoroughly washed with water and a mild soap. Usually, there is a time lapse of approximately 30 to 120 minutes for the furocoumarins to be absorbed into the skin.10 To avoid further exposure to sunlight, the affected skin should be covered for the next 48 to 72 hours. Regular use of broad-spectrum sunscreens may help to prevent or diminish the cutaneous effects of phytophotodermatitis.
Management
In the acute stage, treatment is mainly symptomatic. Mild cases may not require treatment. Cool compresses and topical corticosteroids may be used to reduce local inflammation. NSAIDs can be used for pain relief. More severe cases may require meticulous burn wound care.
No treatment is necessary for the subsequent hyperpigmentation as it usually fades over time. The use of over the counter topical 4% hydroquinone or a prescription modified Kligman’s formulation will hasten resolution of the hyperpigmentation.
Alexander K.C. Leung, MD, is a clinical professor of pediatrics at the University of Calgary and pediatric consultant at the Alberta Children’s Hospital in Calgary, Alberta, Canada.
Benjamin Barankin, MD, is the medical director and founder of the Toronto Dermatology Centre in Toronto, Ontario, Canada.
References:
1. Ozkol HU, Akdeniz N, Ozkol H, et al. Development of phytophotodermatitis in two cases related to Plantago lanceolata. Cut Ocu Toxicol. 2012;31(1):58-60.
2. Klaber R. Phytophotodermatitis. Br J Dermatol. 1942;54:193-211.
3. Kung AC, Stephens MB, Darling T. Phytophotodermatitis: bulla formation and hyperpigmentation during spring break. Mil Med. 2009;174(6):657-661.
4. Zhang R, Zhu W. Phytophotodermatitis due to Chinese herbal medicine decoction. Indian J Dermatol. 2011;56(3):329-331.
5. Abali AE, Aka M, Aydogan C, Haberal M. Burns or phytophotodermatitis, abuse or neglect: confusing aspects of skin lesions caused by the superstitious use of fig leaves. J Burn Care Res. 2012;33(6):e309-e312.
6. Rademaker M, Derraik JGB. Phytophotodermatitis caused by Ficus pumila. Contact Dermatitis. 2012;67(1):47-57.
7. Sarhane KA, Ibrahim A, Fagan SP, Goverman J. Phytophotodermatitis. Eplasty. 2013;
13:ic57.
8. Wagner AM, Wu JJ, Hansen RC, et al. Bullous phytophotodermatitis associated with high natural concentrations of furocoumarins in limes. Am J Contact Dermatitis. 2002;13(1):10-14.
9. Zhang RZ, Zhu WY. Phytophotodermatitis due to wild carrot decoction. Indian J Dermatol Venereol Leprol. 2011;77(6):731.
10. Carlsen K, Weismann K. Phytophotodermatitis in 19 children admitted to hospital and their differential diagnoses: child abuse and herpes simplex virus infection. J Am Acad Dermatol. 2007;57(5 suppl):S88-S91.


